HOW CAN WE HELP YOU? Call 1-800-TRY-CHOP
In This Section
Which Bacteria are Responsible for Early-onset Sepsis in Very Preterm Babies?
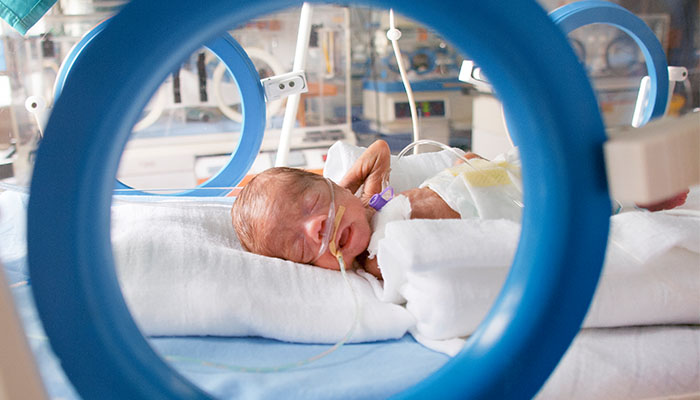
Early-onset sepsis is a significant cause of morbidity and mortality among very preterm infants.
mccannn [at] chop.edu (By Nancy McCann)
The findings:
Researchers at Children’s Hospital of Philadelphia and the Perelman School of Medicine at the University of Pennsylvania set out to determine the epidemiology, microbiology, and outcomes of early-onset sepsis among very preterm infants using a cohort from academic and community hospitals across the United States.
Of the 84,000 infants whose data were analyzed, 1,130 had early-onset sepsis. The most common bacterial pathogen isolated was E. coli, followed by group B Streptococcus, but approximately one-third of infections were due to neither of these organisms. Infants at the lowest gestational ages had the highest incidence of infection. Infected infants had longer lengths of stay, lower rates of survival, and lower rates of survival without morbidity.
Why it matters:
Early-onset sepsis (EOS) is a significant cause of morbidity and mortality among very preterm infants. Because infection epidemiology drives empiric antibiotic decisions by clinicians for the treatment of these tiny patients, updated data on the microbiology of early-onset sepsis was needed. This information can be used to inform empirical antibiotic guidance, highlight risk factors for infection, and aid in prognostication for infected infants.
Who conducted the study:
Dustin D. Flannery, DO, MSCE, a core faculty member in the Clinical Futures, a CHOP Research Institute Center of Emphasis, was first author. Clinical Futures colleague Karen M. Puopolo, MD, PhD, and other collaborators from the University of Vermont and the Vermont-Oxford Network (VON), a nonprofit voluntary collaboration of healthcare professionals who care for neonates, also contributed to the study.
How they did it:
As a prospective observational study of very preterm infants born in 2018 and 2019, the researchers used data collected by VON from 753 hospitals in 49 states. These infants were born weighing less than 1,500 grams and had early-onset sepsis, defined as a culture-confirmed bacterial infection of the blood or cerebrospinal fluid in the first three days after birth.
Quick thoughts:
“The results of this study have important implications for clinicians who assess EOS risk and choose empiric antibiotics for very preterm infants and who counsel families both before and after very preterm birth,” Dr. Flannery said. “The profoundly negative impact of EOS on very preterm infants highlights the need for novel preventative strategies.”
Where the study was published:
The study appears in Pediatrics.
Want to learn more?
Check out this LinkedIn post by the Clinical Futures.


