HOW CAN WE HELP YOU? Call 1-800-TRY-CHOP
In This Section
Recognizing the Complexities in Healthcare: Q&A With Halley Ruppel, PhD, RN

Halley Ruppel, PhD, RN. Photo courtesy of AAMI Conference and Expo 2017.
Editor’s Note: With the World Health Organization’s (WHO) designation of 2020 as “Year of the Nurse and the Midwife,” we took this special opportunity to recognize the community of nurse scientists at Children’s Hospital of Philadelphia. Throughout the year, we featured nurse researchers in a series of Q&As that touched on everything from their research projects to the unique perspective of nurse scientists. This Q&A with Halley Ruppel, PhD, RN, a newly hired nurse scientist and core faculty member in the Clinical Futures, a CHOP Research Institute Center of Emphasis, and Research Assistant Professor at Penn Nursing, is the final installment of the series. We are proud to share the valuable work and wisdom of our CHOP nurse scientists! In case you missed previous posts in this series, read more about Margaret McCabe, PhD, RN, PNP; Ruth Lebet, PhD, RN; Warren Frankenberger, PhD, RN; Elizabeth Froh, PhD, RN; and Amy Jo Lisanti, PhD, RN.
Welcome to CHOP! Can you tell us how long have you been a registered nurse?
Thank you! I have been a registered nurse for 12 years. I also have a master’s degree in Nursing Education and a PhD in Nursing Science.
When did you start to integrate research into your career as a nurse, and why?
I began my career practicing in pediatric critical care. We routinely integrated research findings into practice. Our goal was to provide evidence-based care to our patients. I became interested in conducting research because I wanted to participate in generating knowledge to support nursing practice, so I went back to school for a PhD.
What is your area of focus, and why did you choose that as your research specialty?
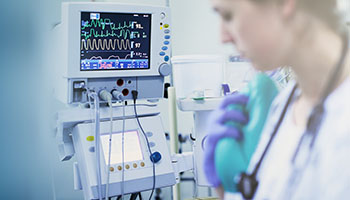
Dr. Ruppel studies the appropriate integration of technology into the care environment with the goal of optimizing patient safety and outcomes.
I am interested in the appropriate integration of technology into the care environment with the goal of optimizing patient safety and outcomes. I was motivated to study technology use because the inpatient care environment is not always conducive to healing and recovery — it’s bright, loud, and often chaotic, especially in the ICU. Advances in technology are exciting but necessitate considerations about the impact on clinician workflows, patient safety, and the care environment.
One of my specific areas of interest is nurses’ use of monitoring technology. Monitoring is a key component of nursing practice; we monitor patients for the effectiveness of interventions, for complications of procedures, for improvement or deterioration, etc. Bedside physiologic monitors are helpful tools, but they have also introduced excessive and often uninformative alarms into the care environment.
By some accounts, there are nearly 200 physiologic monitor alarms per patient per day in the ICU, most of which do not require intervention. Nurses develop alarm fatigue, which is a patient safety risk, and there is likely an opportunity cost to the time nurses spend managing uninformative alarms. Alarms also have potential negative implications for noise levels in the care environment and for stress and sleep among patients and families.
Has your clinical practice influenced your nursing research, or vice versa in any way, and how so?
Yes! Every ICU is full of alarms not just from the bedside physiologic monitors, but also from infusion pumps, ventilators, and other technologies. Most nurses know the experience of being overwhelmed by excessive alarms at one point or another. But we don’t have to normalize the noise and information overload — there are many potential solutions, some that still need to be developed and others that just require a systematic approach to implementation and evaluation.
Can you tell me about some of your current research projects, or research that you’re excited to work on?
In some of my previous work, I have considered how nurses adjust alarm limit settings for individual patients, to better reflect vital sign deviations that would indicate an important change in the patient’s condition. I am interested in continuing to study how to better ensure alarm limit settings are adjusted to be meaningful for individual patients, and the association with reduced alarms and enhanced patient safety.
I am also interested in how we can better use longitudinal alarm data, for example, how many alarms patients have had in the past few hours, to learn and make improvements to the alarm management system. Some of the most influential research on clinical alarms in pediatrics has been done at CHOP, led by Dr. Chris Bonafide, and I am looking forward to continuing to collaborate with his team as well.
Great! Can you tell us more about your additional research interests?
Having experienced the transition from documenting on paper to using the electronic health record (EHR), I am also interested in how the EHR affects clinician workflows and critical thinking processes. I was a postdoctoral fellow in delivery science and informatics at Kaiser Permanente Northern California Division of Research, where I studied clinicians’ navigation of the EHR and use of EHR data for risk prediction to support clinical decision making in women’s health, specifically in the prenatal period.
Why do you think the unique perspective of nurse scientists is so integral to pediatrics and pediatric research? What unique approach do nurse scientists bring?
Just as nurses bring a unique perspective to clinical teams, they also bring a unique perspective to research. In pediatrics, that nursing lens is grounded in patient and family-centered care. From the perspective of my own research in the inpatient setting, most direct-care nurses spend 8- or 12-hour shifts working exclusively with a few patients. Nurses individualize care for these patient and families based on ongoing assessment, intervention, and evaluation, and they form unique relationships with the patients and families. Nurses also recognize the complexities, limitations, and opportunities of the systems in which they work. As a nurse scientist, I bring this perspective to my research to generate knowledge that supports nursing practice in this context.
All researchers bring a disciplinary perspective, whether from nursing or another profession, which informs the questions they ask and approaches they take. Especially in healthcare, interprofessional teams strengthen research.
What excites you the most about being a nurse scientist?
The opportunity to improve the hospital care environment — to optimize patient safety and outcomes. I am excited about new technologies that can facilitate nursing practice and optimize children’s outcomes, and at the same time, I want to mitigate the barriers and challenges that nurses face when trying to deliver care. I am also energized by working with scientists from different professional backgrounds and seeing how our complementary perspectives lead to better questions and more interesting approaches.
What’s in store for you in terms of future research? What do you hope to accomplish?
My long-term goal is to improve the care environment so that there is less noise and more useful information delivered to nurses, and other clinicians, when they need it. My ultimate goal is optimized patient safety and outcomes for children in the hospital.


