HOW CAN WE HELP YOU? Call 1-800-TRY-CHOP
In This Section
MOMS2 Research Reveals Fetal Surgery Benefits Continue to Childhood

Audrey became Children’s Hospital of Philadelphia’s 1,000th fetal surgery patient on March 7, 2013. Six years later, she is “proud and fearless.”
By Nancy McCann
Loud and proud, first-grader Audrey Rose sings to the music of her favorite teen idol. Like other 6-year-old girls, Audrey imitates JoJo Siwa right down to the signature hair bow. Audrey loves dancing: ballet, jazz, and tap are among her favorite styles. Riding a scooter is a mastered skill. Riding a bike is her next conquest. Climbing, swinging, and running around the playground with her classmates is an everyday occurrence; however, unlike her elementary school peers, Audrey has myelomeningocele (MMC), the most severe form of spina bifida.
MMC is a central nervous system birth defect that causes the fetus’ spinal cord and surrounding nerves to protrude from the back. Continuous bathing of the developing spinal cord in amniotic fluid over the course of gestation can result in progressive neurologic injury. Common complications are paralysis of the lower legs, significant bowel and bladder problems, orthopeaedic malformations such as clubfeet, and hindbrain herniation, which can cause fluid on the brain requiring a shunt to relieve the buildup.
So how did Audrey bypass the most severe symptoms of this disorder? She had fetal surgery to repair spina bifida and close up her back before birth — a scar she wears proudly, said Audrey’s mother, Jackie Oberio (See video). On March 7, 2013, Audrey became Children’s Hospital of Philadelphia’s 1,000th fetal surgery patient.
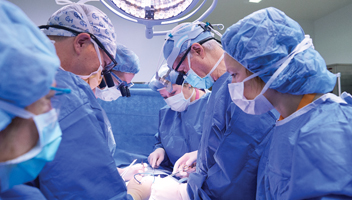
CHOP Surgeon-in-Chief, Scott Adzick, MD, MMM, and team performing fetal surgery at the Center for Fetal Diagnosis and Treatment.
Pioneering surgeons led by Scott Adzick, MD, MMM, CHOP’s Surgeon-in-Chief, first performed this delicate surgery in 1998 at CHOP’s Center for Fetal Diagnosis and Treatment. Since then, the Center, of which Dr. Adzick is founder and director, has continued to improve the technique, leading to significant advances.
New Findings Help to Inform Families
Results from the “MOMS2: Follow-up of the Management of Myelomeningocele Study,” published in Pediatrics, show significant physical and emotional benefits in school-age children — just like Audrey — who received corrective surgery in the womb for MMC.
“These findings add to the growing body of literature demonstrating the benefits of prenatal surgery for spina bifida,” said Dr. Adzick, coauthor of the study and professor of surgery at the Perelman School of Medicine at the University of Pennsylvania. “Caregivers should take these findings into account when counseling expectant mothers to ensure that families considering prenatal surgery for their fetus understand the potential risks and benefits.”
In 2011, results of the original landmark study “MOMS: Management of Myelomeningocele Study” also led by Dr. Adzick, appeared in the New England Journal of Medicine. They showed prenatal repair of spina bifida improved mobility, increased the likelihood of a child walking independently, and greatly reduced the need for a shunt to divert fluid from the brain, as compared to babies who received surgery after birth. The study followed children for two and a half years after surgery.
Now, after following those same two groups of children for up to 10 years after birth, researchers in the follow-up MOMS2 trial, have shown benefits continue into childhood.
Although there was no significant difference between surgery groups in overall adaptive behavior or cognitive benefits, motor function and quality of life were better among children in the prenatal surgery group. Long-term gains included improved mobility and independent functioning in school age children. Walking unassisted, better gross and fine motor skills, improved bladder and bowel control, and fewer surgeries for shunt placement and revision were among the benefits. In addition, the children and families in the prenatal group reported less stress on the family overall, resulting in better quality of life.
“It is extremely gratifying to see that the positive results from the initial MOMS trial endure into childhood,” Dr. Adzick said. “Fetal surgery is a complex and serious procedure and should only be done by experienced teams. Research needs to continue to refine the technique in a way that will improve outcomes even further.”
MOMS2 Study Details
The original MOMS study sought to enroll 200 children, but the National Institutes of Health ended the trial early, after 183 operations, as there was clear evidence of efficacy for the prenatal procedure. Of those 183 babies, 161 participated in MOMS2.
The follow-up study involved a single comprehensive visit with the children between June 2011 and April 2017, when they were between the ages of 6 and 10 years old. The children underwent a neurodevelopmental and behavioral evaluation by a psychologist and a physical exam and functioning assessment by a physical therapist. A parent or caregiver completed the Vineland Adaptive Behavior Scales II, which is used to evaluate adaptive behavior through an interview with a study psychologist.
The three centers that participated in the original MOMS trial (CHOP; Vanderbilt University; University of California, San Francisco), along with the independent data-coordinating center at the George Washington University Biostatistics Center, conducted the MOMS 2 study. The Eunice Kennedy Shriver National Institute of Child Health and Human Development provided funding for the research.
Additional CHOP coauthors of the MOMS2 study include Lori Howell, DNP, MS, RN, executive director of the Center for Fetal Diagnosis and Treatment; Mark Johnson, MD, MS; Larissa Bilaniuk, MD; and Nina Thomas, PhD.
As for Audrey, she will soon be off to softball practice with only the aid of her pink and purple ankle-foot orthosis braces. “She’s really killing it,” her mother said. “She’s completely independent. I think that’s why she is so proud and fearless. She knows the important thing is to do it the Audrey way, whatever that looks like.”