HOW CAN WE HELP YOU? Call 1-800-TRY-CHOP
In This Section
Leader, Mentor in Field of Pediatric Critical Care Medicine: Q&A With Robert Berg, MD

Robert Berg, MD
Editor’s Note: Robert Berg, MD, the Russell Raphaely Endowed Chair of Critical Care Medicine and former chief of the Division of Critical Care Medicine at Children’s Hospital of Philadelphia, is the recipient of the 2022 Distinguished Career Award from the American Academy of Pediatrics Section on Critical Care. This award recognizes a senior leader in the field of pediatric critical care medicine who has made significant career accomplishments and contributed to the subspecialty for 25 years or longer post fellowship completion. Dr. Berg is a renowned resuscitation scientist described by his colleagues as a trailblazer and innovator whose work in the lab and many clinical studies has changed the way resuscitation is performed in both children and adults. And with exceptional mentorship, he has helped to develop the next generation of resuscitation scientists. Read on to learn what this lifetime achievement award means to him.
Congratulations on receiving the Distinguished Career Award from the American Academy of Pediatrics Section on Critical Care during the 2022 AAP National Conference and Exhibition in California! What does this award represent to you?
It’s wonderful to receive special recognition from my colleagues and peers. But truly, what it reflects to me is the fruition of the enormous amount of work and effort by myself, and a lot of other people, to make a difference in pediatric critical care and resuscitation science. As I ponder this honor, I think of the many teams that I’ve worked with over the years. I am reminded of the mentors who have taught me so much, and the mentees, colleagues, and friends who have taught me even more. This award is a testament to these teams of extraordinary people who made impressive contributions and major institutions that supported these efforts.
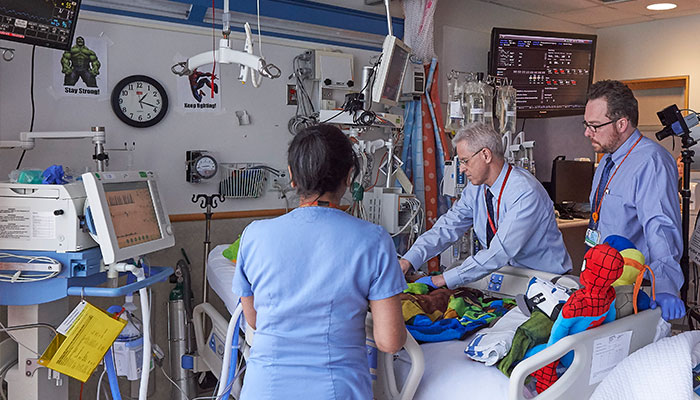
Dr. Robert Berg received a distinguished career award for his innovative contributions to the field of critical care medicine and resuscitation science.
What led you to choose a focus in pediatric critical care?
When I first took care of critically ill children in the 1970s, the survival rate from hypotensive septic shock was about 50%, the survival rate from pediatric acute respiratory distress syndrome (ARDS) was less than 50%, and the survival rate from cardiac arrest was 10%. Using the concepts that my mentors at the University of California San Francisco, taught me about physiology, pathophysiology, pharmacologic principles, I felt we could improve care and save lives.
How do you stay on the cutting edge of your field?
The best way in the world to stay on the cutting edge of pediatric critical care is to be at Children’s Hospital of Philadelphia. Every week, we have multiple conferences and case-based discussions with state-of-the-art intellectual interchange, updating of the most recent information on septic shock, ARDS, fluid management, resuscitation science, renal failure, and more. These conferences include the many international critical care medicine leaders at CHOP, as well as our colleagues in the pediatric subspecialties, surgery and radiology. Of course, we all supplement local learning opportunities with other traditional education, such as keeping up with the relevant medical literature, national and international critical care and resuscitation science meetings, and visiting professorships.

CHOP Critical Care Medicine team
What career achievements and research projects are you most proud of?
As a leader, I am most proud of mentoring and leading the very special CHOP Critical Care Medicine faculty members and trainees for the past 14 years. What I have experienced at CHOP is leading a group of exceptionally talented, impressively bright, and incredibly committed young faculty members. They’ve taught me a lot. It has been a privilege and honor to be part of their career development.
As a pioneer pediatric resuscitation investigator, I am most proud of conceptualizing and confirming the life-saving value of physiologic-directed CPR — first in the laboratory, and then translating these findings from bench to bedside.
As an American Heart Association (AHA) and CHOP Resuscitation Science Center pediatric resuscitation program leader, I am most proud that our AHA guidelines and educational programs have been instrumental in improving rates of long-term survival after in-hospital pediatric cardiac arrests from approximately 10% in the 1980s to close to 25% in 2004 to greater than 50% at CHOP and major children’s hospitals by 2020.
What advice do you have for young physicians and researchers who are beginning their careers?
First of all, have patience. The beginning of a career is really rough across the board, especially academic careers for researchers. The coins of the realm are grants and publications. Only 6% or so of NIH grants get funded, which means getting turned down is the norm. Similarly, the likelihood that a research publication will be accepted at the highest level journals is also less than 10%. So young academic physician-scientists need to experience personally oppressive “failure.” They need to know that short-term failures are OK, that they are normative. So, be patient.
I was advised to always be around people who are smarter, nicer, and better looking than me, and I’ve done that my whole life. Luckily, around CHOP that is easy. Common advice focuses on abundant resources and outstanding mentors — and both are very important. But the secret sauce is really the culture — the people. You want to be in a program with colleagues, mentors, and mentees who are going to help you be the best you can be.
Any additional thoughts?
CHOP has a group of people who are amazing. The breadth and depth of knowledge, experience, and expertise are quite remarkable. The collegial environment is equally impressive. When I visit other institutions, I am easily reminded that I have been quite fortunate to be at CHOP, an extraordinary institution with exceptional people.


