HOW CAN WE HELP YOU? Call 1-800-TRY-CHOP
In This Section
CHOP Academy for Resuscitation of Children — a Heartening Endeavor
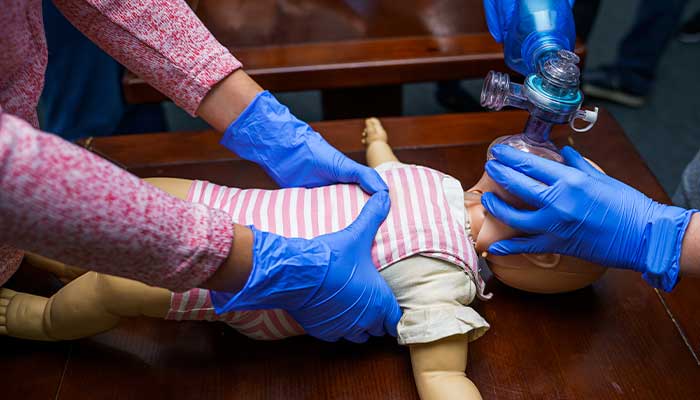
CHOP Academy for Resuscitation of Children aims to improve pediatric in-hospital resuscitation outcomes.
mccannn [at] email.chop.edu (By Nancy McCann)
When a child’s heart arrests, they’re usually very young — 1 to 3 years old, with single system problems, such as respiratory failure. Reversing the problem and resuscitating the child can give them an additional 60 to 70 quality-of-life years. That’s a lot of living to do and why resuscitation science is so important in pediatrics.
Currently in development at Children’s Hospital of Philadelphia is the Academy for Resuscitation of Children (ARC), the implementation science wing of the Resuscitation Science Center, led by Robert Sutton, MD, MSCE, and Todd Kilbaugh, MD, both internationally recognized experts in pediatric cardiac arrest. It’s here, where the next generation of interventions are being discovered to improve survival and outcomes for children.
As an in-person and virtual international training center, ARC will adapt, implement, and disseminate evidence-based resuscitation guidelines to 50 healthcare centers around the globe that are part of the Pediatric Resuscitation Quality Collaborative (pediRES-Q), a clinical learning laboratory network of which CHOP is the clinical, data, and program coordinating center. With pioneering innovation and research, exceptional training, extraordinary care, and genuine collaboration, ARC will support this new Global Resuscitation Alliance with the first 10-step approach to high performance pediatric in-hospital resuscitation practice.

Vinay Nadkarni, MD
“The chances of survival following in-hospital pediatric cardiac arrest ranges from 10% to 70%,” said ARC’s Founding Director Vinay Nadkarni, MD, a leading critical care and resuscitation science researcher at CHOP. “Most healthcare organizations have limited expertise, capacity, and systems of care to efficiently measure and improve how they recognize, prevent, prepare for, and treat pediatric cardiac arrests and clinical emergencies. ARC will bring us closer to eliminating disparities in outcomes by providing evidence-based, optimal resuscitation practices in hospitals in communities all over the world.”
CHOP is the Spot
The Academy for Resuscitation of Children has evolved organically at CHOP, as many globally recognized key leaders of the science of resuscitation have coalesced on CHOP’s campus over the years. As key contributors and leaders of the International Liaison Committee on Resuscitation (ILCOR), these experts continuously review the world’s literature on evolving studies of resuscitation science, help develop the American Heart Association (AHA) evidence-based guidelines on CPR and resuscitation, and create and develop next generation resuscitation tools. CHOP investigators have long collaborated with the Laerdal Foundation, Zoll Medical, Resuscitation Quality Improvement Partners, and the AHA to improve the quality of resuscitation practice and will continue to do so, as ARC will partner with these organizations.
With this collective expertise and experience, CHOP became the ideal place to house ARC, as no such global resuscitation alliance or resuscitation academy model exists for children.
“Here at CHOP, the Academy will be able to test and train to best practices that have been developed in our translational lab, put into guidelines by our clinical research, and then subsequently disseminated through the training provided by ARC,” Dr. Nadkarni said.
Ten-step Global Resuscitation Alliance Model
From pre-arrest, intra-arrest, and post resuscitation care, the Academy has identified 10 elements that are all important to the excellent resuscitation and support of children. The goal is to visit the hospitals within the pediRES-Q network or help to bring hospital personnel to CHOP to figure out where they are among each of the 10 steps and how CHOP can support them in improving the implementation of the best science, the best training, and the best implementation within their hospital.
Working to implement elements such as just-in-time training or spaced learning, which is pulling the information and training needed, right before it’s needed. Take for instance rolling refreshers. These involve rolling a cart that includes a mannequin, defibrillator, and a trainer right outside the room of a sick child who is at risk of arrest and providing a refresher lesson for the care providers every six weeks to three months.
Or perhaps it’s measuring real and simulated resuscitation performance by collecting defibrillator, monitor, and live-capture data; conducting performance debriefings immediately post-arrest for timely feedback to providers and leadership; as well as long-term follow-up at three- and 12-month intervals post discharge.
“There’s much to learn from what the barriers and facilitators are at each of these contexts at each hospital,” Dr. Nadkarni said.
A Beacon Shedding, Spreading Excellence
Information from the learning healthcare system feeds into the data coordinating center at CHOP so the researchers can start to understand what works and what doesn’t for each of these hospitals worldwide. For instance, considering a lower-middle-income resourced hospital environment: What is the best configuration of a code blue team? What are the tools that might be most useful? Can these lower-middle-income resourced centers be matched up with each other to start talking about what works and what doesn’t?
“We’re not just focused on the problems,” Dr. Nadkarni said, “it’s also important to understand the success factors and collect that information in a scientific way — and share it. We envision ARC to be a beacon, shedding and spreading excellence in the hopes of improving pediatric resuscitation outcomes so our youngest patients have the opportunity to enjoy many more quality-of-life years.”
In addition to Drs. Sutton, Kilbaugh, and Nadkarni, Robert Berg, MD; Alexis Topjian, MD; Ryan Morgan, MD; Aaron Donoghue, MD; Neethi Pinto, MD; Dana Niles; Kelly Papili RN; John Erbayri; Anne Ades, MD; Elizabeth Foglia, MD; and Heather Wolfe, MD, MSHP, will contribute their expertise to the Academy.