HOW CAN WE HELP YOU? Call 1-800-TRY-CHOP
In This Section
Identifying Biomarkers as Precursors to Vision Loss in Pediatric OPGs

Dr. Robert Avery is using precision imaging to identify biomarkers for vision loss in children with optic pathway gliomas.
droseyb [at] email.chop.edu (By Barbara Drosey)
Optic pathway gliomas (OPGs) grow in the bundle of the million plus wires, or axons, of the anterior visual pathway that span from the optic nerve through the optic tracts, making them impossible to surgically remove without also destroying vision. Clinicians take a watch-and-wait approach with these low-grade gliomas that can cause vision loss in children, typically between the ages of 1 and 8, but they need a more precise method to detect looming damage to the visual system.
Whereas in most diseases, tumor growth leads to negative outcomes, that’s not always the case with low-grade gliomas like OPGs, which do not behave like typical tumors. These tumors may or may not cause vision loss; may get bigger and not cause vision loss; or may stay the same size and cause vision loss.
“It seems counterintuitive, but in these cases, growth doesn't necessarily mean an intervention is necessary,” said Robert Avery, DO, MSCE, pediatric neuro-ophthalmologist at Children’s Hospital of Philadelphia.
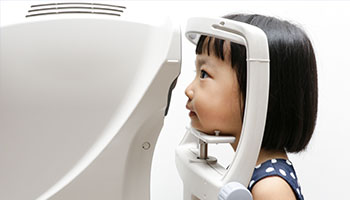
Optical coherence tomography can help determine biomarkers for vision loss.
In his studies using optical coherence tomography (OCT), a noninvasive ophthalmologic imaging test, Dr. Avery is hoping to get a detailed picture of OPGs’ progressive damage and characterize biomarkers to guide treatment decisions. The current standard of care is to initiate chemotherapy after vision loss is detected.
“The current standard of care is akin to waiting for a problem to happen before treatment begins, which is not optimal,” said Dr. Avery, who is also an assistant professor of Ophthalmology and Neurology at the University of Pennsylvania Perelman School of Medicine. “We don’t want to wait until the child has lost vision to start therapy. Also, as long as a child’s vision is stable and these biomarkers look good, we would not want to subject that child to chemotherapy.”
Utilizing OCT, Dr. Avery measures the circumpapillary retinal nerve fiber layer (cpRNFL) and ganglion cell-inner plexiform layer (GCIPL) thickness to determine signs of impending trouble with visual acuity and visual field. The primary hypothesis of his project, “Biomarkers of Vision Loss in Children With Optic Pathway Gliomas,” supported by a $600,000 grant award from the National Eye Institute, is to demonstrate a correlation between magnitude and location of cpRNFL and GCIPL thickness to visual function. Dr. Avery thinks OCT will demonstrate that these measures decline shortly before visual function does, thereby identifying an optimal treatment window and opening opportunities for earlier intervention.
“The beauty of optical coherence tomography of the eyes is we're able to do very high resolution imaging,” Dr. Avery said. “We're achieving tissue-level definition of the cells and axons of the visual system at a resolution of about three microns – to put this in perspective, a red blood cell is about six or seven microns.”
This precision imaging is what Dr. Avery and his team anticipate will enable the identification of the very gradual and specific biomarkers that denote the tipping point of vision loss for children with OPGs. CHOP has recruited about 100 study participants with a goal of 300. Patients receiving routine, clinical care comprise the majority of study subjects, with a majority of the procedures from the study protocol part of their standard of care.
Dr. Avery first developed an interest in this challenging disease during his clinical training. As a well-recognized referral center, CHOP treats a high volume of patients with OPGs. He saw how the disease created frustrations for patients and families, but also identified an opportunity to improve clinical care and outcomes.
“This has potential to be the largest optic pathway glioma study due to the multisite collaboration, and will have an immediate impact on the clinical care, visual outcomes, and diagnostic monitoring of children with OPGs,” Dr. Avery said.
CHOP collaborates and shares data with Boston Children’s Hospital and University of Toronto’s Hospital for Sick Children. Dr. Avery also appreciates the insights of his CHOP colleagues: Michael Fisher, MD, chief of neuro-oncology at CHOP and professor of Pediatrics at the Penn Perelman School of Medicine, Grant Liu, MD, pediatric neuro-ophthalmologist and professor of neurology and ophthalmology at Penn Perelman School of Medicine, and Jeffrey Berman, PhD, CHOP researcher and research assistant professor of Radiology at Penn Perelman School of Medicine.
In addition to providing insight into the mechanism of vision loss related to OPGs, Dr. Avery aims to identify future opportunities for neuroprotective and visual restoration strategies by helping determine how biomarkers such as photophic negative response, visual evoked potential, diffusion tensor imaging, and volumetric MRI change for children who experience visual recovery or visual loss after undergoing OPG treatment. He will expand on this work as principal investigator on a recent grant award from the National Cancer Institute to study quantitative MRI for pediatric OPG treatment response.