HOW CAN WE HELP YOU? Call 1-800-TRY-CHOP
In This Section
A Day in the Life of a Clinical Research Coordinator
 Editor’s Note: Our clinical research coordinators at Children’s Hospital of Philadelphia are a unique professional hybrid. Part researcher, healthcare professional, data coordinator, social worker, personal coach, and travel concierge, they go above and beyond their job descriptions in order to help families navigate the complexities of participating in clinical research studies. We invited Joshua Zigmont, RN, BSN, who has been a nurse research coordinator for seven years, to describe a typical day on the job. The first thing he told us is that the most consistent thing about the position is its inconsistency: “You have to be flexible because you never know when a curveball is coming,” Zigmont said. So while no day is ever typical, here is a glimpse of a day in the life of a clinical research coordinator.
Editor’s Note: Our clinical research coordinators at Children’s Hospital of Philadelphia are a unique professional hybrid. Part researcher, healthcare professional, data coordinator, social worker, personal coach, and travel concierge, they go above and beyond their job descriptions in order to help families navigate the complexities of participating in clinical research studies. We invited Joshua Zigmont, RN, BSN, who has been a nurse research coordinator for seven years, to describe a typical day on the job. The first thing he told us is that the most consistent thing about the position is its inconsistency: “You have to be flexible because you never know when a curveball is coming,” Zigmont said. So while no day is ever typical, here is a glimpse of a day in the life of a clinical research coordinator.
8:00 p.m. Slumber Party Setup
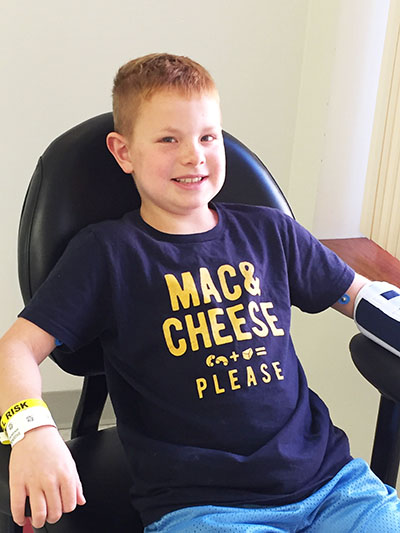 It’s been an all-day marathon — literally, I’ve already tracked 24,000 steps today — and my next research volunteer, 10-year-old Jack Broderick, has arrived at the Center for Human Phenomic Science. CHPS is our home base for conducting many of our clinical research studies at CHOP. Since the studies that I’m currently working on are rather complex, the kids I see get to know this place pretty well. They come here for research visits on about a monthly basis, sometimes less and sometimes more, which allows me to personally connect with the families and offer them a support system. It’s my favorite part about being a clinical research coordinator.
It’s been an all-day marathon — literally, I’ve already tracked 24,000 steps today — and my next research volunteer, 10-year-old Jack Broderick, has arrived at the Center for Human Phenomic Science. CHPS is our home base for conducting many of our clinical research studies at CHOP. Since the studies that I’m currently working on are rather complex, the kids I see get to know this place pretty well. They come here for research visits on about a monthly basis, sometimes less and sometimes more, which allows me to personally connect with the families and offer them a support system. It’s my favorite part about being a clinical research coordinator.
Jack is enrolled in a phase 2 industry-sponsored drug trial that aims to promote muscle regeneration and maintenance for children with Duchenne muscular dystrophy, regardless of the type of genetic mutation that is underlying their disease. He’s been enrolled in the study for about six months, and the research protocol requires him to stay overnight in the main hospital once every three months so that we can perform continuous blood draws to measure the amount of drug that is absorbed by his system. We also monitor his heart and check his vital signs throughout the night to be on the lookout for any possible side effects.
Jack and his mom, Jocelyn, have traveled from Marlton, N.J., and they’ve come prepared to make the sleepover as fun as possible. His bag is packed with his favorite snacks, gadgets, and mini hand trampolines to bounce balls back and forth the small room. It’s not really required that I be here to get Jack settled in, but I realize that spending the night at the hospital is a big commitment for families, so I don’t mind devoting some time to hang out with them. We play games, talk with funny French accents, and then get the “Angry Birds” movie queued up before I head home. We have a busy morning ahead of us.
9:30 a.m. Tackling the Checklist
I’ll be with Jack and Jocelyn throughout the day to make sure they’re where they need to be and that all of their questions are answered. The backbone to keeping the day running smoothly is to schedule everything in advance. I have calendars on top of calendars. Today’s checklist has18 “must do’s.” So that things don’t get too overwhelming for Jack, we’ve come up with a reward system. For each “must do” that we check off, Jack earns a letter. By the end of the day, we’ll spell out “Macaroni and Cheese!” and Jack will get to enjoy his favorite meal.
Jack has already had his morning dose of the study drug, so next on the list is an electrocardiogram to measure his heart’s electrical activity. We start joking around in our French accents again, which makes it hard for him to stop laughing, but Jack manages to keep still long enough, only moving his eyebrows up and down a few times like a comedian and giving a sly grin.
10 a.m. Physical Therapy: Playing can be Hard Work
 It’s not uncommon for me to encounter other departments who aren’t always familiar with the process of clinical research studies. I make the extra effort to establish a good rapport with my colleagues and educate them about why I’m showing up all the time with our young research volunteers. Obviously, they’re busy seeing clinical patients too, so again, scheduling a time that is convenient for everyone is essential. This morning, a physical therapist who knows the research ropes and has worked with Jack before is ready for our visit with an enthusiastic welcome.
It’s not uncommon for me to encounter other departments who aren’t always familiar with the process of clinical research studies. I make the extra effort to establish a good rapport with my colleagues and educate them about why I’m showing up all the time with our young research volunteers. Obviously, they’re busy seeing clinical patients too, so again, scheduling a time that is convenient for everyone is essential. This morning, a physical therapist who knows the research ropes and has worked with Jack before is ready for our visit with an enthusiastic welcome.
We try to keep things fun. Jack goes through a series of tasks such as standing and jumping on one foot, lying down and sitting up, and stacking a tower of cans. His family gave consent for his physical therapy testing sessions to be videotaped for training purposes so that other study sites can learn from our physical therapists’ techniques. I get to be the cameraman, and we pretend to be shooting a movie. Jack gets a kick out of raising his eyebrows as a flourish for the camera each time he accomplishes a task. Next, I grab an office chair for Jack to sit in and wheel him to the starting point of his six-minute walk test. Jack walks a loop up and down the corridor, and I follow behind to ensure the timing and distance is measured as precisely as possible.
Jack is a fifth-grader and still very able-bodied despite his diagnosis, so he usually can get through the physical therapy exam in about 30 minutes. But the study he is enrolled in has an age range of 5 to 10 years old, so it can take much longer when I’m dealing with younger kids. That’s why it’s so important for me to have a good relationship with the family. I’ve learned the ins and outs of how to work with each child and know some tricks get them to do the testing when they’re flat out not cooperating. Some children with Duchenne muscular dystrophy are sensitive to certain sounds and textures, so taking their shoes off for the physical therapy exam can be challenging. I often end up taking my shoes and socks off as well to convince them that it’s cool to be barefoot.
10:45 Back for a Blood Draw
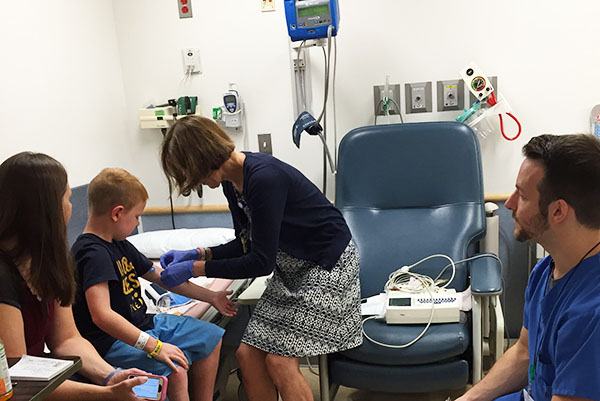 We head back to Jack’s room at the CHPS for another blood draw. Jack is a pro at this part, and a clinical research nurse easily takes care of him and collects the blood sample, although I’m always willing to jump in. One benefit of having a nursing background and being a clinical research coordinator is that I can pull double duty whenever needed, getting labs drawn or taking vital signs, those sorts of things. The CHPS staff appreciates it very much when I can help out if they’re swamped.
We head back to Jack’s room at the CHPS for another blood draw. Jack is a pro at this part, and a clinical research nurse easily takes care of him and collects the blood sample, although I’m always willing to jump in. One benefit of having a nursing background and being a clinical research coordinator is that I can pull double duty whenever needed, getting labs drawn or taking vital signs, those sorts of things. The CHPS staff appreciates it very much when I can help out if they’re swamped.
While Jack is in good hands, I take a moment to double check all of the data I’ve gathered so far this morning. Tracking everything takes a lot of time and attention. My job is to stay tuned to any little symptom or issue that is going on, and then to document the entire clinical study day. By tomorrow, I’ll have all of the data that I collected from Jack’s visit entered into the system of the pharmaceutical company conducting the study, and someone there will review it with a fine-tooth comb to ensure it’s accurate.
11:15 Taking a Breath
It’s always a relief to have the blood draws out of the way. Now, we’re off to cross the bridge that connects to the hospital’s new outpatient facility, the Buerger Center, a colorful, curvy building with a swirling walkway that Jack loves to follow. I let the front desk of the pulmonary function testing department know we’ve arrived. The technician is working on calibrating the machines for Jack’s testing, so we have a few minutes to relax. Jack and I sit next to the window with a view of the Buerger’s Center rooftop garden below us, and he shows me his latest video game.
While being a buddy isn’t necessarily on my job description, I always try to consider the child’s outlook on things. For them, they’re told by their parents that being on a study is to help them, but being here all day for these visits can be boring and tedious. I’ll always find a few minutes during the day to take an interest in what they’re reading, drawing, playing on their computer, etc. Building that connection can go a long way.
The pulmonary function testing is a bit of a workout for Jack. He performs a series of breathing maneuvers, and everyone in the room tends to follow the instructions too: “Suck the air in as hard as you can, now blow out with a big blast … go, go, go, keep going!” Jack gets a new “high score,” and gives a big smile.
Noon: Why Take Part in Clinical Research?
 As we head back to the CHPS for Jack’s well-deserved lunch break, Jocelyn talks about why she finds participating in clinical research so valuable: “Being in a study gives a lot of hope for families. There’s much to be gained and nothing to be lost. Here at CHOP, they take all the pressure off your shoulders. They are top-notch professionals who keep you informed every step of the way, and the more you find out about how the research process works, the less intimidating it is.”
As we head back to the CHPS for Jack’s well-deserved lunch break, Jocelyn talks about why she finds participating in clinical research so valuable: “Being in a study gives a lot of hope for families. There’s much to be gained and nothing to be lost. Here at CHOP, they take all the pressure off your shoulders. They are top-notch professionals who keep you informed every step of the way, and the more you find out about how the research process works, the less intimidating it is.”
It’s good to hear her put into words what I try to accomplish each day. For me, being a nurse and a clinical research coordinator as well, I’m often the first point of contact for families who volunteer for these neuromuscular studies. They’ll reach out with research questions, clinical questions, and sometimes they’ll reach out with social work questions too. They’re seeing me so often, and they’re so used to talking to me, that I really get to know them.
Even though it’s a lot of work, it’s also one of the things that I find most satisfying about my job. I put myself in the shoes of these families. They have a lot on their plates, and the severity of their children’s diagnoses comes with a lot of mental stress. When they offer their children to be participants in these studies, I think that commands a certain amount of dedication and sense of compassion as a clinical research coordinator to go the extra mile and make things as fun, easy, and enjoyable as possible.